Understanding the symptoms of type 2 diabetes is essential in order to identify the condition and seek appropriate medical attention. By being aware of these signs, you can take proactive steps towards managing and potentially preventing further complications associated with this condition. In this article, we will discuss the symptoms of type 2 diabetes, both common and uncommon, that you should be aware of.
What Is Type 2 Diabetes?
Type 2 diabetes is a chronic condition characterised by the body’s inability to use insulin efficiently or gradually losing the ability to produce enough insulin. Insulin is a hormone that helps regulate the levels of glucose (sugar) in the blood. When insulin is not used effectively, glucose levels in the blood can become too high.
Insulin resistance is a key factor in the development of type 2 diabetes. It occurs when the body’s cells do not respond properly to insulin, leading to an accumulation of glucose in the blood. Over time, this can cause the pancreas, which produces insulin, to work harder and eventually lose its ability to produce enough insulin.
The Symptoms of Type 2 Diabetes
Common Symptoms
- Frequent urination (polyuria)
- Increased thirst (polydipsia)
- Increased hunger (polyphagia)
- Fatigue or tiredness
- Blurred vision
- Slow-healing sores or frequent infections
- Unintended weight loss
- Tingling, pain, or numbness in the hands or feet (neuropathy)
Less Common Symptoms
- Darkened skin (acanthosis nigricans)
- Frequent yeast infections or UTIs
- Dry, itchy skin
- Erectile dysfunction in men
- Reduced sensation or numbness in the extremities
- Loss of hearing
- Patches of shiny, tight skin (digital sclerosis)
- Changes in the amount or appearance of body and facial hair (in women)
Rare Symptoms
- Delayed stomach emptying (Gastroparesis) causing nausea, vomiting, bloating, and a feeling of fullness even after eating just a small amount of food
- Progressive degeneration of a weight-bearing joint (Neuropathic Arthropathy)
- Painful and hard-to-move shoulder (Adhesive Capsulitis)
- Firm, yellow, pea-like bumps on the skin (Eruptive Xanthomatosis)
- Disabling pain, from peripheral neuropathy
Recognising the symptoms of type 2 diabetes is crucial for early detection and effective management.
Excessive thirst and frequent urination are common signs of type 2 diabetes. When blood glucose levels are consistently high, the kidneys try to rid the body of excess glucose by producing more urine, leading to increased trips to the bathroom.
Blurred vision may also occur as a result of high blood glucose levels. Diabetes can affect the blood vessels in the eyes, causing fluid to leak into the lens and distorting vision. Numbness or tingling in the hands or feet, known as peripheral neuropathy, is another symptom of type 2 diabetes.
Fatigue is often experienced by individuals with type 2 diabetes, as the body’s cells struggle to effectively utilise glucose for energy. Slow-healing wounds, recurring yeast infections, and increased hunger can also be indicative of the condition. Unexplained weight loss may occur due to the body’s inability to properly use glucose and break down fats for energy.
In some cases, certain skin disorders like acanthosis nigricans, which causes dark, thickened patches of skin, may also be present. Additionally, individuals with type 2 diabetes may have a higher susceptibility to infections.
If you experience any of these symptoms, it is recommended to consult with a healthcare professional for further evaluation and diagnosis. Early detection and management of type 2 diabetes can significantly improve long-term health outcomes.

Are The Symptoms of Type 2 Diabetes The Same in Children?
Yes, the fundamental symptoms of type 2 diabetes are generally the same in children as they are in adults. However, the presentation and recognition of these symptoms might vary based on age, maturity, and other factors. Here are the symptoms of type 2 diabetes in children:
Common Symptoms of Type 2 Diabetes in Children:
- Frequent urination (polyuria): A child might start wetting the bed after a history of nighttime dryness or need to go to the bathroom more frequently during the day.
- Increased thirst (polydipsia): The child may seem to be constantly thirsty and drink large quantities of water.
- Increased hunger (polyphagia): Despite eating regular meals, the child might still report being hungry.
- Fatigue: The child may seem more tired or lethargic than usual.
- Blurred vision: While children might not always articulate this symptom, they may squint or express difficulty reading or seeing things clearly.
- Slow-healing sores or frequent infections: Cuts, bruises, or infections that take longer than usual to heal.
- Unintended weight loss: Despite consuming more food due to increased hunger, the child might still lose weight without trying.
- Tingling, pain, or numbness in the hands or feet: While this is more common in adult populations, children might still experience these neuropathic symptoms.
Other Indicators in Children:
- Acanthosis nigricans: Darkened and thickened patches of skin, especially in the armpits, neck, or groin areas. This is a significant indicator in children and can be a clue for doctors that the child might be at risk for or have type 2 diabetes.
- Mood changes and irritability: Some children may become more moody or irritable due to fluctuating blood sugar levels.
- Poor school performance: Unexpected drops in academic performance or concentration could be indirect indicators of the disease.
It’s important to note that while children can develop type 2 diabetes, it was once considered very rare. However, with increasing obesity rates and lifestyle changes, the incidence of type 2 diabetes in children is rising. If there is any suspicion of diabetes in a child, it’s crucial to see a paediatrician or primary care provider for evaluation.

Types of Diabetes
There are various types of diabetes, including type 1 diabetes, type 2 diabetes, and gestational diabetes.
Type 1 diabetes is an autoimmune disease where the immune system mistakenly attacks the insulin-producing cells in the pancreas. As a result, the body is unable to produce insulin, a hormone necessary for converting glucose into energy. Type 1 diabetes is usually diagnosed in childhood or early adulthood and requires regular insulin injections for survival.
Type 2 diabetes, on the other hand, is the most common form of diabetes, accounting for approximately 90% of cases. It occurs when the body becomes resistant to insulin or fails to produce enough insulin to maintain normal blood sugar levels.
Gestational diabetes, which affects pregnant women, is a temporary condition that increases the risk of developing Type 2 diabetes later in life.
There are also less common types of diabetes, such as type 3c diabetes, LADA (Latent Autoimmune Diabetes in Adults), MODY (Maturity-Onset Diabetes of the Young), neonatal diabetes, and brittle diabetes. These types have different underlying causes and characteristics, which may vary from person to person.
Understanding the different types of diabetes is crucial for proper management and treatment. If you suspect you have diabetes, it is important to consult a healthcare professional for an accurate diagnosis and customised care plan.
What Are the Causes of Type 2 Diabetes
Type 2 diabetes is primarily caused by a combination of genetic and lifestyle factors. While genetics play a role in determining an individual’s risk of developing the condition, certain lifestyle choices can significantly increase the likelihood of developing type 2 diabetes.
- Genes: Certain genes can predispose individuals to insulin resistance, a condition in which cells do not effectively use insulin. Insulin is responsible for transporting glucose from the bloodstream into cells to be used as energy. When cells do not respond properly to insulin, glucose builds up in the blood, leading to high blood sugar levels.
- Weight and Obesity: Carrying excess weight, especially around the waist, increases the risk of developing insulin resistance. Excess fat tissue can release chemicals that interfere with the body’s ability to use insulin effectively. Furthermore, obesity is often associated with other metabolic abnormalities, such as high blood pressure and high triglyceride levels, which further increase the risk of developing type 2 diabetes.
- Metabolic Syndrome: Metabolic syndrome refers to a cluster of conditions, including high blood sugar levels, high blood pressure, high triglyceride levels, low HDL cholesterol levels, and excess abdominal fat. Metabolic syndrome increases the risk of developing insulin resistance and type 2 diabetes.
- Liver Glucose Production: In individuals with type 2 diabetes, the liver may produce too much glucose. Normally, the liver releases glucose into the bloodstream to maintain healthy blood sugar levels. However, in people with type 2 diabetes, this process is dysregulated, leading to elevated blood sugar levels.
- Communication Issues Between Cells: Type 2 diabetes can also occur when there are communication issues between cells in the body. Insulin normally signals cells to take in glucose from the blood. In individuals with type 2 diabetes, this communication between insulin and cells is impaired, leading to high blood sugar levels.
- Malfunctioning Beta Cells: Beta cells in the pancreas are responsible for producing insulin. In some cases of type 2 diabetes, beta cells do not function properly, resulting in insufficient insulin production.
Other risk factors for type 2 diabetes include:
- Age: The risk of developing type 2 diabetes increases with age. People over the age of 45 are more susceptible, although it can occur at any age.
- Ethnicity: Certain ethnicities, including African Americans, Hispanic/Latino Americans, American Indians, and Asian Americans, have a higher risk of developing type 2 diabetes. This could be due to a combination of genetic and lifestyle factors.
- Medical History: Having certain medical conditions, such as prediabetes, polycystic ovary syndrome (PCOS), gestational diabetes during pregnancy, or a history of heart disease, can increase the likelihood of developing type 2 diabetes.
Understanding these risk factors is essential for early detection and prevention. Adopting healthy lifestyle choices, such as maintaining a balanced diet, engaging in regular physical activity, and managing stress levels, can reduce the risk of developing type 2 diabetes and its complications. Regular check-ups, blood tests, and monitoring of blood sugar levels are also recommended for individuals with risk factors, allowing for early intervention and improved quality of life.
Type 2 Diabetes Diagnosis and Tests
Early diagnosis of type 2 diabetes is crucial for effective management and to prevent complications. If you are experiencing symptoms such as excessive thirst, frequent urination, unexplained weight loss, fatigue, or blurry vision, it’s important to be evaluated for diabetes. Testing for type 2 diabetes involves a variety of blood tests to measure the levels of glucose in your blood.
One commonly used test is the A1c test, which measures your average blood sugar levels over the past three months. Another test is the fasting plasma glucose test, which measures your blood sugar after fasting for at least eight hours. In some cases, an oral glucose tolerance test (OGTT) may be recommended, where your blood sugar is measured before and after consuming a glucose drink.
It’s important to note that a diagnosis of type 2 diabetes is typically confirmed through multiple blood tests. This is because the results can vary, and it’s important to ensure accuracy. Your healthcare provider will analyse the results and consider your symptoms and medical history before making a diagnosis.
Type 2 Diabetes Treatment
Treating type 2 diabetes involves a combination of lifestyle changes and medications. The goal of treatment is to manage blood sugar levels and prevent complications.
Weight loss is often recommended as excess weight can contribute to insulin resistance. Losing even a small amount of weight can have a significant impact on blood sugar control. A healthy eating plan, with a focus on balanced meals and portion control, helps regulate blood sugar levels. Regular exercise, such as aerobic activities and strength training, improves insulin sensitivity and helps manage weight.
In addition to lifestyle changes, medication may be prescribed to help control blood sugar levels. Metformin, a commonly prescribed medication, helps lower glucose production in the liver and improves insulin sensitivity. Sulfonylureas stimulate the pancreas to produce more insulin. GLP-1 receptor agonists stimulate insulin secretion, suppress glucagon production, and promote satiety.
In some cases, combination therapy may be necessary. This involves using two or more medications to achieve optimal blood sugar control. In advanced cases, when other treatments are insufficient, insulin therapy may be needed to control blood sugar levels effectively.
Treating type 2 diabetes is a lifelong commitment. Regular monitoring, self-care, and adhering to the prescribed treatment plan are vital for maintaining good blood sugar control and preventing complications. Working closely with healthcare professionals can help individuals with type 2 diabetes lead a full and healthy life.
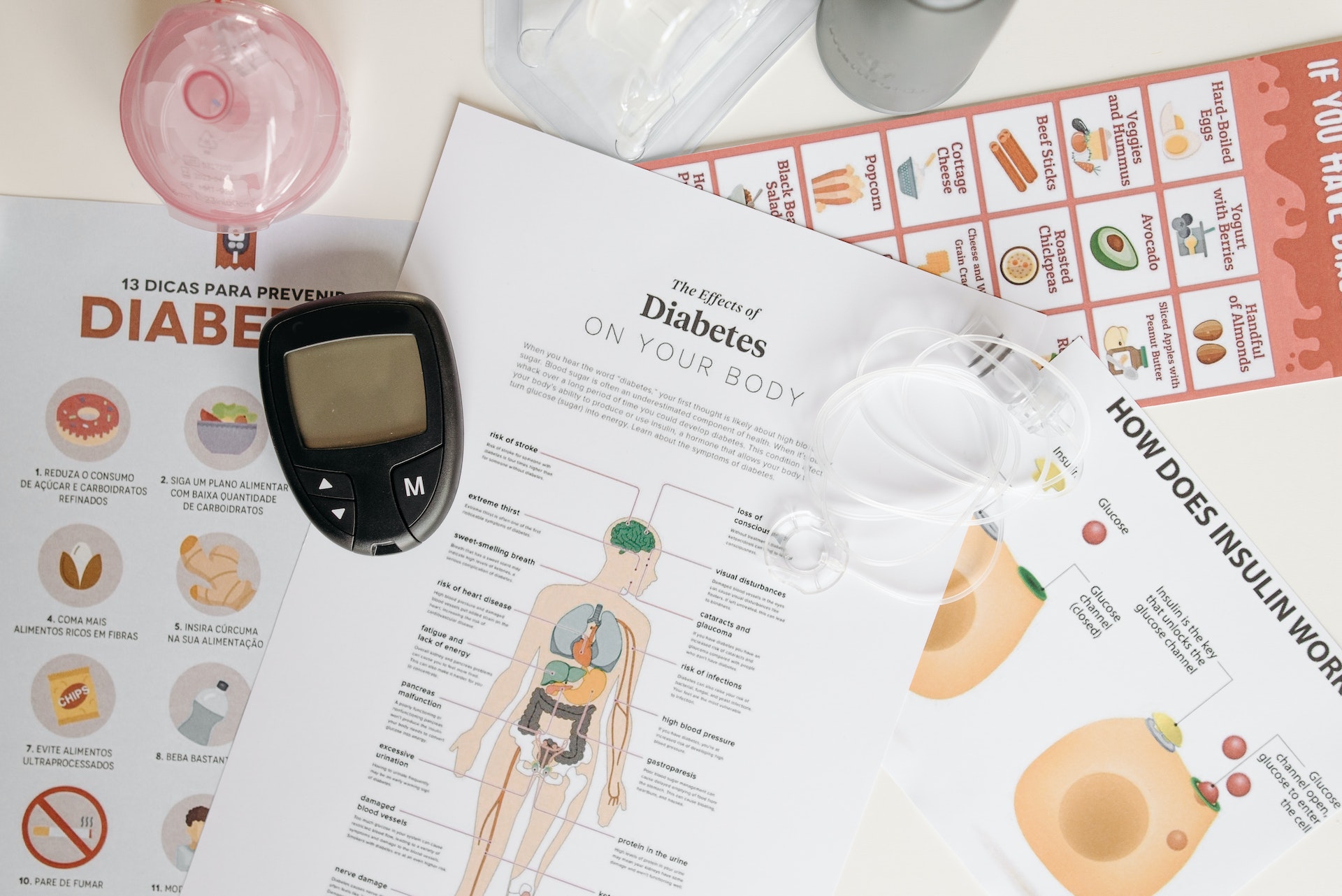
Type 2 Diabetes Complications
Type 2 diabetes can lead to a range of health issues that affect various parts of the body, such as the heart, blood vessels, kidneys, eyes, nerves, and skin. Additionally, women with type 2 diabetes may face complications during pregnancy.
Heart disease is a significant concern for people with type 2 diabetes. The condition increases the risk of developing heart disease and experiencing heart attacks and strokes. Similarly, damage to blood vessels can lead to poor circulation, increasing the risk of conditions such as peripheral artery disease.
Diabetic kidney disease, also known as diabetic nephropathy, can result in kidney failure. High blood sugar levels can damage the kidneys over time, affecting their ability to filter waste from the body effectively.
Diabetic retinopathy is an eye disease that can cause blindness if not adequately managed. Nerve damage, known as diabetic neuropathy, can result in tingling, numbness, or pain in the hands, arms, feet, or legs. This condition can also lead to problems with digestion, sexual function, and urination.
People with type 2 diabetes have a higher risk of developing sleep apnea, a sleep disorder marked by pauses in breathing during sleep. They are also more prone to hearing problems and are at an increased risk of brain damage due to reduced blood flow to the brain. Depression is another complication associated with type 2 diabetes, with studies suggesting a bidirectional relationship between the two conditions.
Fortunately, there are steps individuals can take to manage type 2 diabetes effectively. This includes taking prescribed medications as directed, checking blood sugar levels regularly, following a balanced diet, engaging in regular physical activity, and maintaining a healthy body weight.
Type 2 Diabetes Prognosis
While there is currently no cure for type 2 diabetes, individuals can achieve blood sugar control through weight loss, healthy lifestyle changes, and medication, potentially leading to the discontinuation of diabetes medications.
The long-term outlook for people with type 2 diabetes depends on their ability to manage the condition effectively. Uncontrolled high blood sugar can lead to various complications. However, by reducing A1c levels, quitting smoking, and lowering LDL cholesterol, individuals can significantly lower their risk of these complications and improve their life expectancy.
While living with type 2 diabetes can present challenges, it is important to prioritise your health by following a comprehensive management plan and attending regular check-ups with your healthcare team. By taking proactive steps to manage your condition, you can significantly improve your long-term prognosis and overall quality of life. Some research even shows that type 2 diabetes can be reversed, if the necessary lifestyle changes are made.
As with all conditions, prevention is better than management! Fortunately, preventing type 2 diabetes is highly achievable. Research has shown that losing weight can cut the risk of developing type 2 diabetes by a staggering 50 percent. Incorporating physical activity into your daily routine, such as getting active for at least 30 minutes a day, can reduce the risk by almost a third.
Conclusion
In conclusion, being aware of the symptoms of type 2 diabetes is crucial for early detection and management of the condition. By recognising the signs such as frequent urination, increased thirst, unexplained weight loss, and fatigue, individuals can seek medical attention and receive the necessary treatment to prevent further complications.
It is important to remember that symptoms may vary from person to person, and consulting with a healthcare professional is always recommended for proper diagnosis and personalised care. With early intervention and lifestyle modifications, individuals with type 2 diabetes can lead healthy and fulfilling lives.

Personalised Nutrition for Type 2 Diabetics
For many with Type 2 diabetes, losing weight can be a beneficial step towards better health. But, figuring out the most suitable way to achieve this isn’t always straightforward. Everyone’s journey and challenges with nutrition and dieting are as distinct as their fingerprints.
Fortunately, whether you’re navigating the complexities of diabetes or simply want to improve your overall well-being, our diet matchmaking eBook offers a deeper understanding of personalised nutrition tailored for individuals like you.
What’s Inside:
- Recognizing 26 Challenges: Addressing common and unique hurdles individuals face on their weight loss journey.
- Exploring 11 Diet Plans: Uncover which method aligns best with your health goals and diabetes management.
- Interactive Diet Exploration: A tailored exercise to help pinpoint a nutritional approach suited to your needs.
- 2-Week Meal Plans for Each Diet: Begin your journey confidently with structured and easy-to-follow meal plans.
Over 200 pages of guidance available for just £3.99.
Your journey to better health shouldn’t be a generic template. Let our guide assist you in overcoming obstacles, whether you find challenges in emotional eating, need flexibility with cheat days, lack culinary skills, or face other unique barriers. With our eBook, find the tailored path that respects and supports your individuality.